[ad_1]
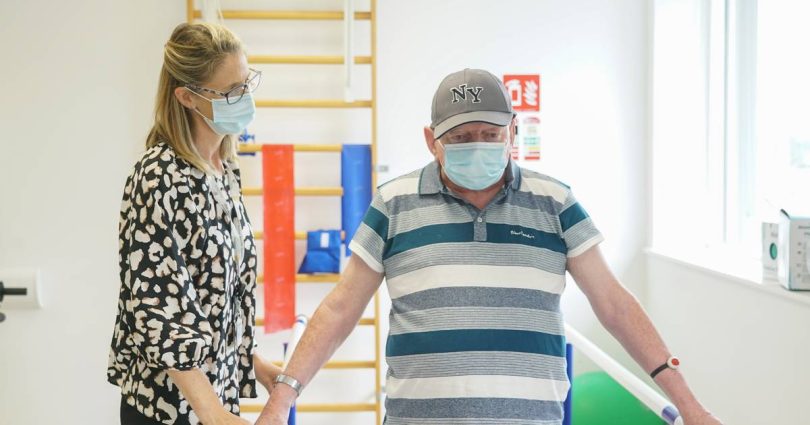
Four months ago, Charles Reynolds was chair-bound and unable to lift a cup of tea or feed himself. But after receiving physiotherapy in his community, he is walking again and feels like he has regained his life.
The 79-year-old spent nine weeks in hospital last year and was diagnosed with heart failure, Parkinson’s disease and epilepsy.
“When Charles came home from the hospital he wasn’t able to walk, he wasn’t able to do anything,” his wife Joyce said. “They advised me that I wouldn’t be able to look after him because I was the same age as him.
“And they said he’s not able to walk so I wouldn’t be able to do it. I went up to him one day and he was crying in the hospital and I asked what’s wrong. He said that they wanted him to go to a nursing home. So I said, ‘No, you’ll never go to a nursing home, don’t take any heed of that’.”
Joyce brought Charles home but struggled to care for him, saying she lost two stone trying to carry him around the house.
Eavan Lennox, senior physiotherapist at the Bray Primary Care Centre, began to visit their home in March. She assisted Charles with “simple, chair-based exercises”, before they eventually progressed to standing exercises. Had the service not been provided locally, he would have been required to attend hospital twice a week for six weeks.
Charles said he has almost returned to normality since then. “I should be dead,” he added. “It gave me my life back.”
Charles was one of the first patients to receive treatment through the Bray Primary Care Centre, which opened in May. It is a part of the Enhanced Community Care (ECC) programme, a core part of the Sláintecare forms, which seeks to reduce pressure on services and dependence on the acute hospital system at a time when record numbers are attending emergency departments and on waiting lists.
To date, 83 of the 96 community healthcare networks have been established, with 2,000 of the target of 3,500 additional staff recruited.
The Bray facility also offers services including a breastfeeding clinic, mental health facility, adult speech and language therapy, dentistry and a voluntary meals on wheels service. The mental health clinic has a project called Parc, which aims to reduce waiting times for psychosocial interventions and assessments for those with mild to moderate mental health disorders.
Ann Cunningham, advanced mental health nurse practitioner at the clinic, said the result has been no waiting lists for psychiatric assessment, psychosocial assessment or for mental health nursing. “You get seen and you’re offered an intervention the following week. We know that qualitatively this works,” she said.
The pilot project also found that 60 per cent of patients recovered and 28 per cent of patients improved following Parc’s interventions, she said.
Speaking at the facility on Wednesday, Minister for Health and local TD Stephen Donnelly said these care centres are the “future of healthcare”.
“When we talk about moving care out of hospitals, people avoiding hospitals or only in extreme circumstances, this is what we’re talking about,” he said.
“Expert teams in the community, advanced nurse practitioners, nurses, we have an awful lot of specialists here, working together, working across disciplines and supporting patients directly.”
[ad_2]
Source link