[ad_1]
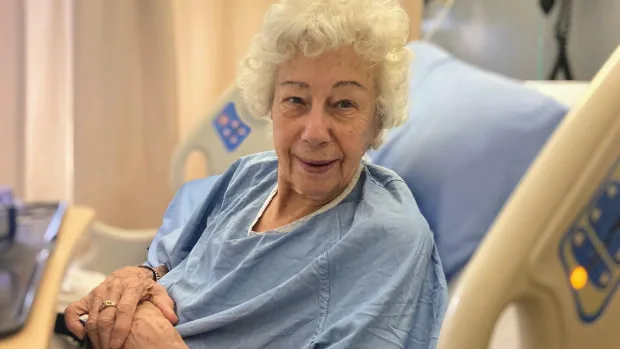
At the age of 87, Gladys Sibley’s biggest regret in life, as she faces her final years, is that she isn’t spending this time with people who love her.
Her parents died when she was young and, in rural Nova Scotia, she raised her siblings like she was their mother.
Since then, she separated from her husband and became estranged from her children and extended family.
I started training to become a doctor in 2020 and met Gladys at the onset of the pandemic through a volunteer program connecting seniors in isolation with students. She allowed me to share her story. We met in person for the first time Sunday, Sept. 4. Before that I called her every week. And those calls changed the way I look at medicine and the way seniors like Gladys, living their final days without family to take care of them, are treated by the health care system.
Gladys says she’s no “negative Nelly” and she’s made it clear she doesn’t want to be anyone’s burden. But it doesn’t take much to see that the system isn’t serving a growing population of seniors. I fear the consequences of a generation of people feeling this way. When Gladys had what we consider a red flag symptom in medicine I encouraged her to seek hospital care. A red flag symptom is usually a sign of a serious condition. The patient should see a doctor or get tests right away. Gladys ended up staying in the hospital for several days and described the experience as de-humanizing, just laying there, waiting for health providers to come by, and no visitors to share the time with.
Don’t grow old, dear.– Gladys Sibley
A year ago, she had to leave her apartment after her health became worse. She moved to a retirement home in Ontario where she lives alone and there, she says, “it’s always about the money”. She says there are added fees when she needs to send documents to her doctor and more fees to access entertainment. A lot of unexpected costs.
I was shocked to hear that a doctor only shows up about twice a month in a retirement home with more than 100 people living there. There is not much I can do. I listen and promise that I will do what I can as a future physician to improve the system.
How Ontario could provide better care for older adults
Dr. Amit Arya, a palliative care physician who works in long-term care homes, is an advocate for improving care for seniors. He says “part of the problem is our hospital system, and our health care system was not at all designed to look after the needs of older adults. It was built … at a time when our population was a lot younger. And that’s why the Canada Health Act only includes physician care, the kind of care delivered in clinics and includes hospital care.
He says “everything else is outside the Canada Health Act and is not an essential service whether we look at palliative care, home care, long term care, medications, all these things are outside.”
Arya wants to see a system that focuses on keeping older adults aging in place at home, a choice most seniors prefer. He also wants adequate funding for hospital beds, primary care, pharmacare, and homecare. All would prevent seniors from falling through the cracks.
Arya lists four steps the province could take to provide better care for older adults.
1. Housing and food security
Address the social determinants of health such as housing and food security because seniors are one of the fastest growing groups of people who are homeless and living in poverty.
2. Staffing
Ensure adequate staffing in the system that allows enough time to care for seniors. Arya says it’s important to “have enough health workers so that people are not so short staffed and so stretched that they can provide appropriate care to older adults. This is something which takes time”
3. Continuity of care
Arya says “continuity of care is another major issue. So, this is a problem where if somebody doesn’t know you, they don’t know your wishes and values. They don’t know who we are as a person. This is where inappropriate care can often happen.”
4. Training
There is a shortage of people with training and expertise in caring for seniors. He believes that to address this, “we need to ensure that all health workers are trained and have required competencies in geriatrics and in palliative care.”
As the health system currently stands, I worry about its ability to care for seniors like Gladys, my mother, and one day, myself. We need to build a better health system so that our seniors know that they are not a burden, but lives worth cherishing and that society will take care of them regardless of how much family support they have.
As Gladys tells me “don’t grow old, dear.” I wish that could be true.
[ad_2]
Source link